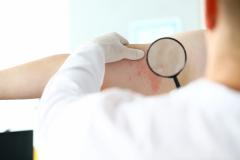
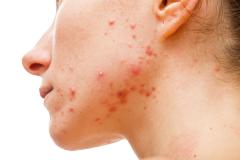
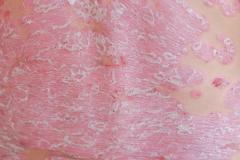
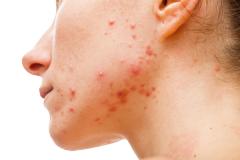
Dr John Harris Outlines the Outcomes of Stopping Treatment With Ruxolitinib Cream for Vitiligo
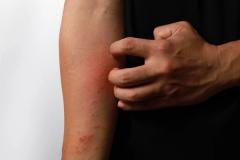
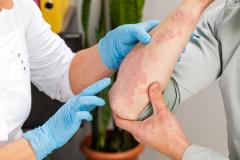
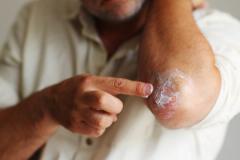
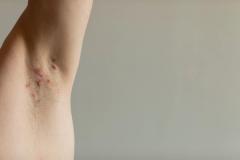
Similar to other therapies, approximately 40% of patients with vitiligo who stopped treatment with ruxolitinib cream relapsed, but they achieved repigmentation once treatment was reinitiated, explained John Harris, MD, PhD, FAAD, director of the Vitiligo Clinic and Research Center at UMass Chan Medical School.
This content was produced independently by The American Journal of Managed Care® and is not endorsed by the American Academy of Dermatology.
Similar to other therapies, approximately 40% of patients with vitiligo who stopped treatment with ruxolitinib cream relapsed, but they achieved repigmentation once treatment was reinitiated, explained John Harris, MD, PhD, FAAD, director of the Vitiligo Clinic and Research Center at UMass Chan Medical School.
At the annual meeting of the American Aca b Dermatology, Harris presented results from the withdrawal arm of the TRuE-V extension study.
Transcript
How long were patients with vitiligo on ruxolitinib cream in the randomized withdrawal arm of the TRuE-V extension study, and what did you find regarding relapse once they were taken off treatment?
We know from published reports that relapse to other typical conventional therapies is about 40% within a year of stopping any treatment for vitiligo. One of the big questions was this new topical JAK [Janus kinase] inhibitor, ruxolitinib, how would it behave and what we would we see in patients? We saw that patients do relapse after stopping the treatment. It appears that the JAK inhibitor doesn't create long-term, durable responses, but it's not any worse, certainly.
When we say 40% of patients relapse within a year, that means 60% don't relapse within a year, and 60% get long-term benefit. We see that with the topical ruxolitinib, as well. Part of that study was to stop patients who had achieved a certain amount of repigmentation—more than 90%, repigmentation—and then either continue to treat them with drug or treat them with placebo and then see how that changes. Then, those who relapsed, put them back on the drug and see how they do.
It was interesting, we certainly saw some relapse—like I said, it was not worse than what we've seen before. When we put them back on drug, they achieved repigmentation again, so there was no tachyphylaxis or lack of response to reinitiation of drug. In some patients, too, we also saw those who continued on drug also could experience some relapse. But the good news is, as they continued on the drug, those that relapsed actually repigmented again.
It appears that there's some dynamic changes that occur, even when drug is continued. That can be seasonal changes. We know that the drug does a little bit better when getting some light. Maybe during summer, they went over the VASI [Vitiligo Area Scoring Index] 90, and then in the winter kind of pulled back a little bit and vacillated. That's one possibility.
But overall, the take-home message is that relapse does occur, but we're able to get great responses again after re-exposure to the drug.
Newsletter
Stay ahead of policy, cost, and value—subscribe to AJMC for expert insights at the intersection of clinical care and health economics.